Introduction
Acknowledgment of the importance of the vascular access nurse and team were obvious at this year’s Association for Vascular Access (AVA) Annual Scientific meeting. When Ramzy Nasrallah took over as CEO for the Association of Vascular Access (AVA) in 2017, he consolidated the mission of AVA “Protect the Patient, Educate the Clinician and Save the Line” to make it more memorable and to create a more powerful message. (See SmartTRAK interview with Nasrallah at AVA 2017). Nasrallah’s ultimate goal for AVA is to be “the biggest, most reputable, and highly regarded healthcare association in the world” with tens of thousands of members globally. Since taking the helm and advancing his agenda…AVA membership has grown by nearly 20%. Not surprising as the Vascular Access discipline can easily document its financial value by demonstrating up to millions in cost savings by reducing the number of central line-associated blood stream infections (CLABSIs) and/or complications and waste associated with peripheral intravenous catheters (PIVs). At Hartford Hospital, Hartford, CT, their vascular access team increased from 7 full time equivalents (FTEs) in 2017 to over 20 FTEs by the end of the year. And, at Emory University Hospital, Atlanta, GA, their team has grown from 5.4 FTEs in 2017 to 15.9 FTEs in 2019.
At this year’s AVA Annual Scientific meeting three areas of clinical study stood out at the meeting demonstrating the value of the vascular access team in practice:
- Reduction of PIV catheter complications and waste through the PIV5Rights Bundle
- Improved catheter securement & stabilization via a novel device, a tissue adhesive
- Implementation of the MAGIC approach to vascular access in the pediatric population
Attention Builds on PIV Complications
AVA 2019 started with an attention getting presentation by AVA CEO, Nasrallah, where he highlighted that data breaches for big companies such as Capital One and Facebook occurred due to “unguarded peripheral routes into their systems.” Nasrallah stressed that patients don’t care if they obtain an infection from a central line or a peripheral line, and that the same scrutiny provided to central lines are needed for peripheral lines as well. Attention to peripheral lines was also boosted this year by ECRI listing “Infection from Peripherally Inserted IV Lines” in its 2019 Top 10 Patient Safety Concerns. ECRI suggests that to reduce the risk of infection a need exists for increased awareness of PIV-catheter-related infections, in combination with routine active surveillance and follow-up reporting.
Research presented at AVA confirmed significant improvements could be made to PIV catheter performance from both a patient & financial perspective. Results from a study done at Hartford Hospital, called the PIV5Rights Bundle were the subject of several presentations and posters at the meeting. Hartford’s vascular access specialty team (VAST) used Lean and Six Sigma methodology to compare standard practice – insertion by the generalist nurse, to a 5-step multimodal best practice intervention strategy designated as the PIV5Rights bundle implemented by its VAST. The Right Approach Bundle, PIV5Rights, consisted of P=Proficiency, I=Insertion, V=Vein and Catheter, 5=Supplies & Technology and R=Review & Assessment. A few key aspects of the bundle were the use of a trained team (VAST), utilizing the right vein, correct catheter size and the use of designated products. As expected a CHG alcohol prep for skin disinfection was utilized, along with a specified catheter, anti-reflux needleless connector and a new-to-the-market CHX antimicrobial, bordered securement dressing. Key items in the assessment and care included assessment of catheter function twice daily, hub disinfection, flushing twice daily, dressing change at 7 days and PIVC maintained by the team until clinically indicated discontinuation. Results for the two groups are provided below in Table 1.
Although cost of supplies increased $2.60 and labor costs were up $2.51 per insertion in the intervention group, the 80% decrease in catheters purchased/used in that group drove the overall costs down dramatically. When these increased costs and the decrease in catheters usage were extrapolated across Hartford Hospital on an annual basis, gigantic cost savings of almost $3MM per year were achieved with the PIV5Rights Bundle. These savings were used to justify an increase in the VAST services at the hospital, increasing the FTEs to over 20 by year-end.
See what SmartTRAK offers in Wound Care Coverage
Companies and products to benefit from implementation of this bundle include:
- Chlorhexidine gluconate/alcohol prep (Becton Dickinson’s ChloraPrep)
- 22g, 1.75” catheter (BBraun’s Introcan Safety)
- Anti-Reflux needleless connector (Nexus Medical’s TKO)
- CHX antimicrobial bordered securement dressing (entrotech life sciences’ PevahexCHX)
The youngest company and newest product on the market, and perhaps the one to gain the most from this study, is entrotech life science with PrevahexCHX, an antimicrobial securement dressing that contains the singular, pure form of chlorhexidine (CHX) – a unique component compared to other products on the market that contain chlorhexidine gluconate (CHG). Entrotech life sciences developed a groundbreaking non-thermal, patented manufacturing process that is able to unlock the true potential of pure CHX. The principal investigator on the PIV5Rights Bundle, Lee Steere, chose PrevahexCHX to: 1) stabilize the catheter with a bordered securement dressing 2) protect the site with an antimicrobial (CHX) that offered rapid onset of action against microorganisms most commonly found at the catheter site and 3) provide the ability to see and assess the site.
With 36,835 catheters estimated to be used at Hartford Hospital on an annual basis and a cost of PrevahexCHX varying between $1.50 for the smaller sizes and $3.00 for the larger sizes, the opportunity for entrotech life sciences’ is significant. However, the big win takes place when the product is used on the over 250 million PIV catheters inserted annually in the US today.
The ability of the Hartford Hospital VAST to achieve 1 PIVC per patient was extraordinary, this work will inspire other vascular access teams to conduct similar studies – ultimately reducing costs, improving patient care and raising the awareness and credibility of the vascular access team.
Novel Securement Device Making Inroads
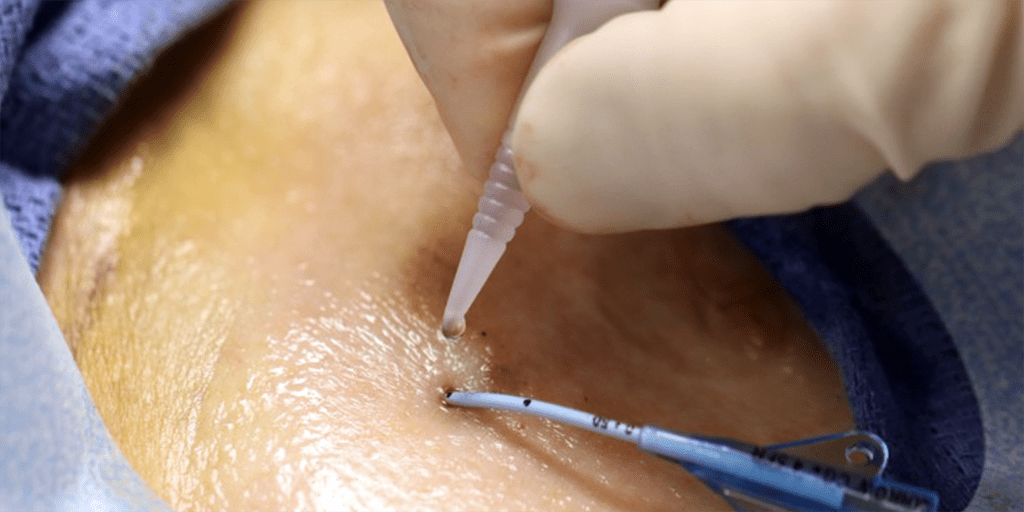
Securement of both central line and peripheral catheters is critical as poor securement can lead to dislodgement, infection and/or phlebitis. The vast majority of products used today for securement include basic film (polyurethane) dressings, film dressings with stabilization and mechanical securement devices. 3M holds the leadership position in dressings with its Tegaderm line of products while BD leads the mechanical securement with its StatLock Stabilization Devices. However, a new class of product is emerging and making inroads in the market with impressive clinical and cost-effectiveness data. Adhezion Biomedical’s SecurePortIV Catheter Securement Adhesive, a cyanoacrylate-based liquid adhesive, provides securement but also seals the insertion site from bacteria and was FDA cleared as a 510(k) Class II medical device in Sept 2017. The opportunity for SecurePortIV adhesive is impressive, at ~$6.00 per insertion site the total market opportunity for PIVs and central lines is estimated by SmartTRAK at $1.5B. With only a 20% adoption rate, a potential of $300MM exists. This opportunity may become a reality for Adhezion Biomedical as SecurePortIV has been the subject of numerous clinical trials demonstrating clinical benefit and cost effectiveness, with several having results presented at the recent AVA meeting.
The oncology/hematology department at the Mayo Clinic Arizona found securement and stabilization of its peripherally inserted central catheters (PICCs) needed improvement. Dr. Joan Ralph Webber, a clinical nurse specialist, reviewed alternative devices associated with securement and stabilization and was impressed with published results associated with tissue adhesive. Webber championed a clinical study to compare the use of SecurePortIV adhesive with a securement dressing to a retrospective cohort using an antimicrobial disc and an engineered stabilization device. One year later, the use of SecurePortIV adhesive demonstrated a decrease in migration rates to 1.4% from 19.35%, no CLABSI’s for 5 consecutive quarters and cost benefits of the tissue adhesive compared to the use of a chlorhexidine disc and engineered securement device. The facility is currently working towards approval for use of SecurePortIV adhesive across all catheter lines.
In another study, Jennifer Thompson, Vascular Access Manager at Texas Health Huguley Hospital Fort Worth South, presented results of four separate study protocols using a variety of products, that were tested to evaluate dressing adherence, moisture presence, skin integrity and average dwell time. The fourth and final protocol had only one item added to the standard protocol – use of SecurePortIV adhesive to the insertion site. Use of SecurePortIV adhesive in the dressing protocol demonstrated an impressive decrease in PIV disruption from 70% to 18% while achieving an 87% completion of therapy rate. A cost analysis determined use of SecurePortIV adhesive will save the hospital $407k of which $204k are material costs. Plans at this facility are to adopt SecurePortIV adhesive for use on all catheters.
Other impressive results were presented from several hospitals including many children’s hospital where benefits were seen in reduced dressing changes, decreased bleeding, lower infection rates and reduced dislodgement. With these impressive results, SmartTRAK talked with Adhezion Biomedical’s Chairman and CEO, Pete Molinaro about next steps moving forward.
Molinaro stated, “Our strategy is to continue to conduct meaningful clinical trials in an effort to expand SecurePortIV adhesive’s claims and further validate the already presented impressive results. We are grateful for the enthusiastic response shown by the vascular access clinical community for this product and gratified to hear that key opinion leaders view SecurePortIV adhesive as the next standard of care.”
Finally miniMAGIC
The Michigan Appropriateness Guide for Intravenous Catheters (MAGIC) made waves when it was published in 2015. The effort was led by Vineet Chopra, MD, MSc and his team, along with a multidisciplinary meeting of global experts. The process for developing criteria used the RAND appropriateness UCLA method to determine use, care and management of PICCs and related vascular access devices in hospitalized patients. The outcome of that work became the foundation for vascular access care bundles to reduce catheter-related blood stream infections and other complications.
At this year’s AVA meeting, a new era of MAGIC occurred with the launch of miniMAGIC for pediatrics, a combination of efforts supported by Michigan Medicine, Griffith University and the AVA Foundation. Current data shows needle sticks per PIVC for complex children is 6 compared to the average of 2, the average dwell time to be only 50 hours and that 50% of these devices fail. In addition, 1 in 4 central venous access devices (CVADs) fail prior to completion of therapy. With this poor performance of vascular access devices in pediatrics, the goal of miniMAGIC is to develop a novel pediatrics algorithm that delivers evidence-based recommendations to improve patient outcomes. The algorithm is to provide excellence in device selection, device characteristics and insertion technique. The group reviewed 1,234 scenarios to develop the miniMAGIC protocol to reduce infection and complications in pediatrics. Final results will be published in 2020.
